How One Stevens Researcher Uses Brain Machine Interfaces to Help Heal Parkinson's and Stroke Patients
Almost one million people each year in the United States experience the debilitating effects of a stroke, according to the American Stroke Association. One of those effects is the loss of hand mobility, meaning everyday tasks like holding a cup of coffee, picking up a fork or fastening a button become impossibly difficult. Rehabilitation is key to restoring that mobility, but it is a long, frustrating and complicated process.
Vrajeshri Patel is working to change that.
A Ph.D. student in the Department of Biomedical Engineering, Chemistry and Biological Sciences at Stevens Institute of Technology, Patel studies how the brain controls complex hand movements. She uses that data to design models used for non-invasive technologies to control hand and upper-limb prosthetics.
Working with assistant professor Ramana Vinjamuri, who built the Sensorimotor Control Laboratory for this purpose, Patel has been researching movement control and learning. "We have an idea of how complex parts like an arm are controlled, but there’s so many details we still don’t know," Patel said.
"My Ph.D. is about analyzing different bio-signals that form motor control," she says. "You can do that through kinematics, meaning how you flex your arm. You can do electromyography or EMG, which are muscle signals. I just began working with electroencephalograms or EEG, which are brain signals. I’ve been hoping to work with EEGs since my Master’s, so I’m doing my most exciting research right now.
Three Different Ways to Combat Hand Disability
One of Patel’s first projects was a custom-built symptom tracker. Working with neurosurgeon Michael Pourfar of NYU Langone Medical Center, Patel built the software to help Parkinson’s patients suffering from micrographia. Micrographia is a side effect of Parkinson's where patient’s handwriting gets smaller as they write, and includes other symptoms like tremor, rigidity and slow movements. "It’s hard to get this type of data in a clinical environment," Patel says. "There are a few systems out there, but they aren’t good at measuring all these symptoms."
In order to help micrographia patients regain fine movement control, Patel outfitted them with a glove and other motion trackers to collect and analyze data from their movements and writing samples. These patients already had deep brain stimulators implanted that alleviated some of their symptoms. The reasons why are unclear, but Patel created diagnostic software to help figure it out.
A neural recording cap with electrodes__.
Patel outfitting electrodes into a neural recording cap.
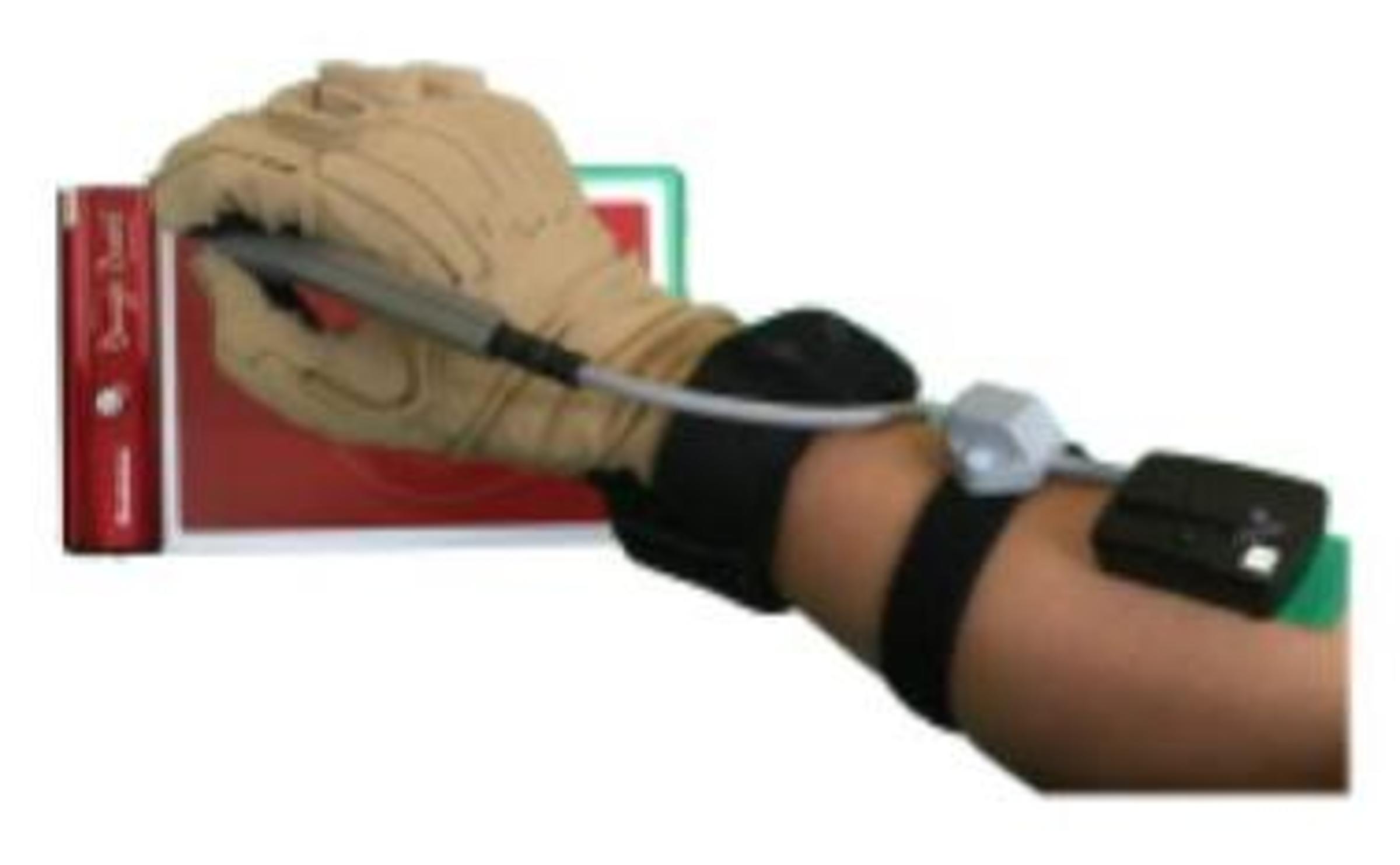
A sensor Patel uses to monitor muscle signals.
Patel puts on the sensor gloves.
Patel using the glove and sensor setup to write. CREDIT: Vrajeshri Patel.
The software adds quantitative analysis to existing qualitative techniques, giving clinicians better real-world feedback—and treatment options. "It’s important to work directly with hospitals to get real-world input from patients and incorporate the doctor’s ideas," Patel says.
Still, it wasn’t easy to create such a complex solution. "This was a very involved project—we did all the recording at the hospital—but it was a lot of fun."
Another project Patel worked on revolved around biometrics, or the use and measurement of human characteristics as identification markers. She summarizes the project: "Can we use hand movements to tell our identity?"
The short answer? Yes.
Using a glove outfitted with sensors and an EEG cap that tracked participants’ brain signals, Patel and Vinjamuri ran an experiment that had subjects grasp "a variety of everyday objects, like cups and pencils" and extracted patterns from those interactions. One pattern they found was that some people extend their index finger further than others. In others, the pinky bends a lot when bending the ring finger. That tiny difference makes it part of a pattern—and a biometric signifier.
Patel demonstrates a grip test with her glove.
GIF of Patel demonstrating the glove and its sensors.
Patel and Vinjamuri applied for a patent for this technology. They also hope to develop it further with commercial funding. That may sound like a reach, but it isn’t for Patel. "I was an Innovation and Entrepreneurship doctoral fellow," she explains, "and in the I&E program they encourage you to think bigger and do more with your research."
Patel is also working with undergraduate student Stephanie Sayegh in the lab to develop virtual reality solutions to help patients. "When we want to teach people how to use their prosthetic, it might be easier to introduce them to an immersive environment first," she explains. The other reason they’re developing the virtual reality environment is for neurorehabilitation, as she says:
Right now, if someone has a stroke and they have some paralysis, they would have to go into a rehab clinic and practice their rehab exercises under supervision. But if they were to do it as part of a game, or while wearing one of our (sensor-outfitted) gloves, we could quantify how well they’re doing, notice their improvements—and give them a little more motivation.
Allowing a patient to perform their rehab in a virtual environment might potentially allow them to do it at home, saving them time and effort—and saving rehab centers resources. "We’ve also come up with some ideas to speed up the re-learning process," she adds. Yet for all those benefits, there are very few virtual reality developments for upper limb prosthetics. "There’s a lot of development in lower limb, but not upper limb," Patel says, for much the same reason there are more lower limb prosthetics than upper limb: "The hand is so complicated." It’s much harder to create and define a virtual reality environment to accurately test all of those factors, much less build one from scratch.
Patel sets up the virtual reality environment.
But the lab has done just that. Right now, they’re testing their virtual reality environment with undergraduate students. They hope to test with patients soon. "I’m really excited to get it running," says Patel.
Building A Path of Her Own
Patel is genuinely excited to move these projects forward; she’s been interested in biomechanical engineering since high school. "I was always interested in the brain and the spinal cord," Patel said. "I thought I could work in this combined field and really go somewhere with it."
But before she could do that, she needed more exposure to neuroscience than her Master’s classes gave her. She contacted Vinjamuri and he started mentoring her, offering advice like "you can find sample data sets here," and "you need to develop these skills in order to be good in the field," she lists.
"Eventually he came to Stevens, and I came as well."
Patel was Vinjamuri’s first lab student, and they built the lab from scratch. "We built the lab together, from ordering computers to figuring out what equipment we needed," she said. "It’s been a roller coaster," she laughs.
"One thing about doing research, even with a mentor, is you have to find your own willpower because you need to push yourself and there will be a lot you need to teach yourself," Patel says. "I knew that coming into the program. But with Vinjamuri as my mentor, he allows me to explore the data, take time with it, and learn how to analyze it. He is the best researcher I have ever met and he respects me as an independent learning researcher."
The Sensorimotor Control Laboratory now has an additional Ph.D. student, Marty Burns, who built a hand exoskeleton controlled by muscle signals and has also been highly essential in building up the lab. There are also two graduate students, and a score of undergraduate students who handle the bulk of the work during the summer. "They’re great,” Patel says. “They’re hard workers and highly motivated and bring a lot of energy to the emerging field of biomechanical engineering."
Everyone is united in helping paralysis patients regain control.
"With biomedical engineering, there’s always going to be a person using our device that we have to serve," Patel says. "Sometimes working across different engineering fields or clinical specialties is difficult. In the end, though, all of our hard work goes toward serving them. It’s completely worthwhile."