These New Nanotech-Powered Bandages & Skin Grafts May Help Heal Your Wounds As They Cover Them
Stevens-Texas A&M team demonstrate promising new material for dressings, grafts that can deliver antibiotics and healing proteins
A Stevens Institute of Technology research team, in collaboration with Texas A&M University, has unveiled a new advance in chronic-wound care that blends advanced materials and nanotechnology with conventional antibiotics and healing proteins.
Biomedical engineering professor Hongjun Wang and his Stevens team helped verify and improve the technology, described in April in the journal Advanced Healthcare Materials.
The new material works like a conventional skin graft, explains Wang — but, in addition to patching a wound in the skin, this material is responsive: it can actively deliver healing proteins and protective antibiotics directly to the surfaces of wounds. Potential medical applications could include advanced dressings for the treatment of chronic wounds, burns, ulcers and sores.
Cleaner wounds, healing more quickly
The Stevens team began by electrospinning a specially designed nanofiber mesh from collagen, polycaprolactone (a biodegradable polymer) and TGF-β1, a human growth-factor protein that speeds the growth and recovery of cells and tissues. Next the Texas team attached micelles — packets of liquid containing one of several antibiotics — to the surfaces of the mesh, where they were slowly released. Packets of antibiotics, the team found, did indeed reduce infection (by Staphylococcus aureus bacteria, in this case).
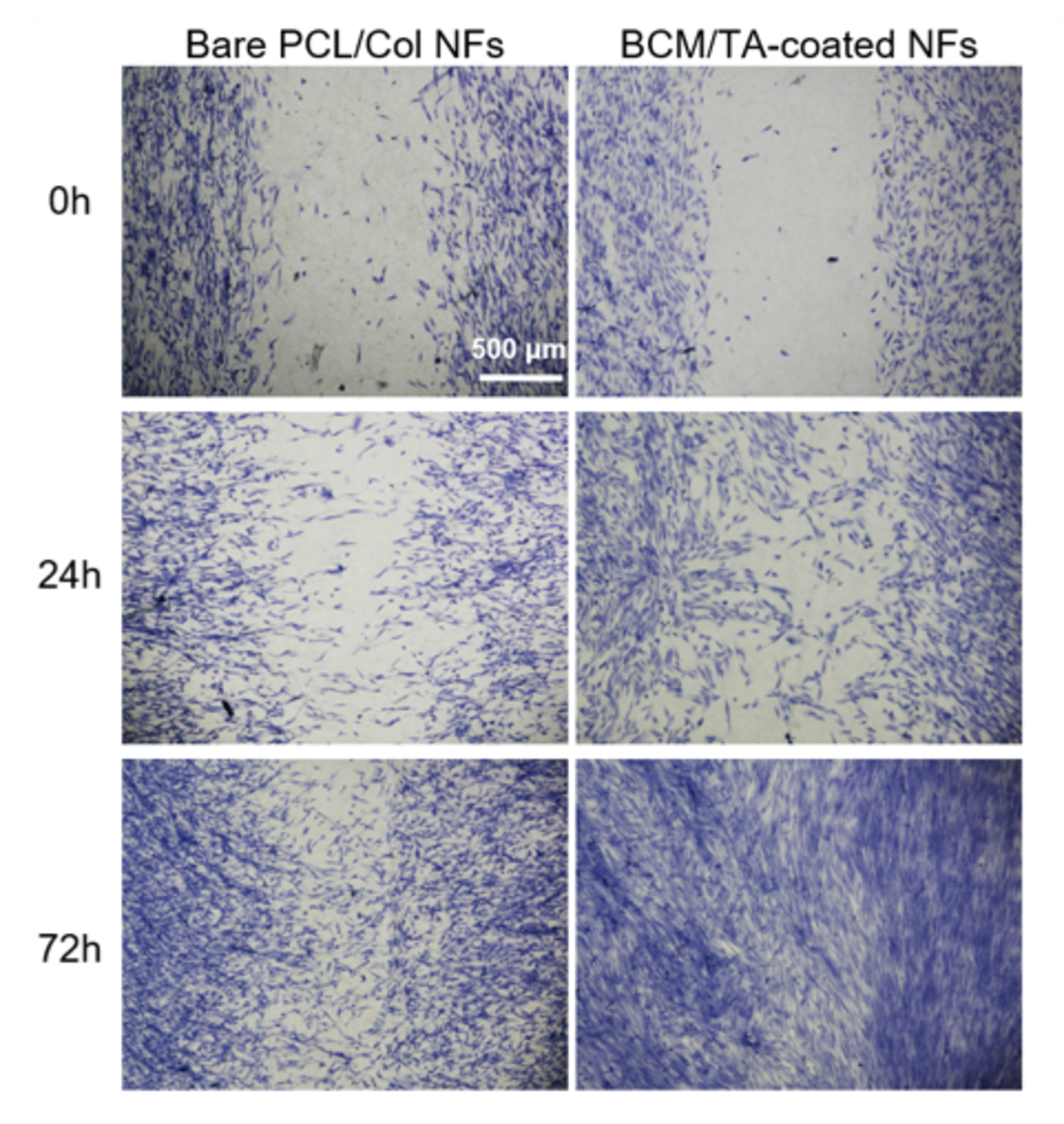
Wang's team then tested the material's properties on human cell cultures in Stevens labs, discovering that the growth factor-infused fibers enhanced fibroblast growth and cellular growth, migration and wound repair compared with non-enhanced fibers.
“This is an important stepping-stone for developing smarter skin grafts that can help facilitate wound healing while minimizing infection for slow-to-heal skin wounds,” notes Wang. "Now that we have shown very promising in vitro results with human cells, the next step is to further demonstrate the concept in vivo with animals and human patients in the future."
The two university teams will continue to refine the graft material, he adds, tailoring it for different types of wounds and working to develop mechanisms that enable programmable delivery of growth factors or antibiotics to wounds in timed doses.